Pediatric Heart Disease Treatment in Northern Virginia & Maryland
Maintaining optimal heart health is crucial for everyone, particularly for children with heart conditions. The Children’s Heart Institute, provides comprehensive care for children with heart diseases. Our team includes a pediatric cardiologist and pediatric sub-specialists who address non-cardiac health issues.
For pediatric cardiology services in Maryland and Northern Virginia, please contact us to schedule an appointment at one of our many pediatric cardiology offices. Our facilities are equipped to conduct pediatric testing and treatment for a variety of heart conditions.
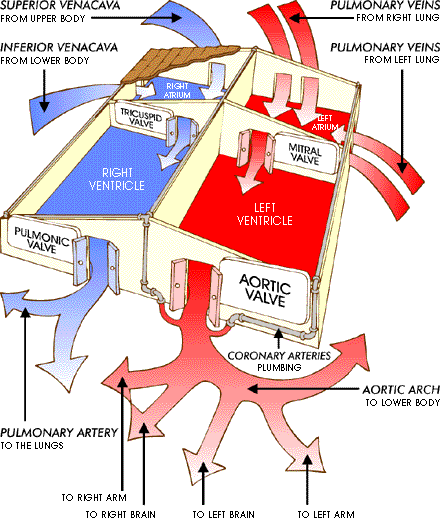
The Anatomy of the Heart
The Heart House analogy helps to understand the normal flow of blood through a healthy heart, which consists of:
- 4 Rooms (Chambers)
- 4 Doors (Valves)
- 4 Big Hallways (Vessels)
- 4 Small Hallways (Vessels)
Let’s explore the potential defects (abnormalities) that can occur within the “heart house” and how they affect a child’s heart.
Congenital Heart Disease
Issues with the Walls:
- Atrial Septal Defect (ASD): A hole between the right atrium and left atrium, treated by patching the hole.
- Ventricular Wall Defect (VSD): A hole between the two ventricles, treated by patching the hole.
- Coarctation of the Aorta: A narrowing of the aorta, which may require surgical intervention.
Pulmonary Artery Issues:
- Branch Pulmonary Artery Stenosis: Narrowing of the pulmonary artery branches.
- Transposition of Great Arteries: Swapping of the two main hallways leading away from the heart, treated with various surgical procedures.
Complex Heart Conditions:
- Tetralogy of Fallot: A combination of four different heart defects.
- Truncus Arteriosus: Missing part of the wall between the front chambers, treated with surgery.
- Common Atrioventricular Canal: A combination of ASD and VSD, treated with surgery.
- Ductus Arteriosus: A persistent passageway between two major arteries, treated with surgery.
Chamber Issues:
- Hypoplastic Right Ventricle: A small and weak right ventricle.
- Hypoplastic Left Heart Syndrome: A small and weak left ventricle.
Plumbing Problem:
Anomalous Origin of the Coronary Artery from the Pulmonary Artery: The coronary artery originates from the pulmonary artery instead of the aorta, leading to cardiomyopathy.
Problems with the Doors
- Tricuspid Valve. The Tricuspid Valve is located between the right atrium and right ventricle. If this door is not developed this condition is called Atresia (Tricuspid Valve Atresia). There is a 3-step procedure to fix this defect:
- Stage 1: Shunt Operation
- Stage 2: Glenn Operation
- Stage 3: Fontan Operation
- Since the door did not develop in the baby before birth there was no blood coming from the right atrium to the right ventricle so the right ventricle became underdeveloped (hypoplastic right ventricle). If the tricuspid door is displaced downward from it’s usual location, this will result in the right atrium becoming excessively large and the right ventricle small and underdeveloped. This condition is called Ebstein Anomaly.
- Mitral Valve. The mitral valve is the door between the left atrium and the left ventricle. If the mitral valve does not develop during the very early gestation weeks, the blood in the left atrium will not flow to the left ventricle, and therefore the left ventricle will be small and underdeveloped (Hypoplastic Left Heart Syndrome). There is a 3-step procedure to fix this defect:
- Stage 1: Norwood Operation
- Stage 2: Glenn Operation
- Stage 3: Fontan Operation
- Pulmonic Valve. The pulmonic valve is the door located between the right ventricle and the main pulmonary artery. If this door is a little bit small (depending on how small it is) we call this condition stenosis (Pulmonic Valve Stenosis). If it does not develop at all we call this condition atresia (Pulmonic Valve Atresia).
- Aortic Valve. The aortic valve is the door located between the left ventricle and the aorta. If the valve is small this condition is called stenosis (Aortic Valve Stenosis). If this valve does not develop at all this condition is called atresia (Aortic Valve Atresia).
Schedule Treatment for Pediatric Heart Disease at the Children’s Heart Institute Today!
If your child has been diagnosed with a heart condition, or if you suspect they may have a heart issue, don’t wait to seek treatment. The Children’s Heart Institute, offers comprehensive care for pediatric heart conditions in Maryland and Northern Virginia. Our experienced team of pediatric cardiologists and pediatric sub-specialists, are equipped to provide the specialized care your child needs. Schedule your child’s appointment at one of our pediatric cardiology clinics in NOVA and Maryland today and ensure they receive the expert care and support they deserve. Call now to schedule your appointment and take the first step towards better heart health for your child.
